[ad_1]
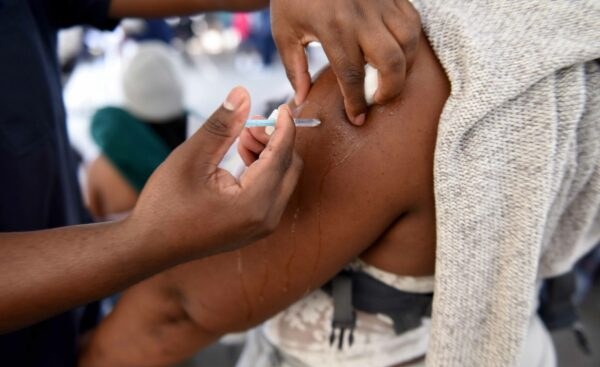
Cape Town — The Covid-19 crisis has highlighted the need for greater investment in Africa’s vaccine manufacturing capacity. The Africa Centres for Disease Control and Prevention (Africa CDC) held a high-level panel which brought together several health experts to discuss how this may be addressed.
Patrick Tippo, with more than 30 years’ experience in the vaccine manufacturing industry, opened the discussion with by lamenting the lack of capacity in Africa’s vaccine manufacturing industry, later going on to say that the continent is at a “make or break” moment in its vaccine manufacturing capacity, but welcomed the work done by the Partnerships for African Vaccine Manufacturing (PAVM) initiative. Tippo worked with BioVac, a private-public partnership in South Africa since its inception in 2003, is currently head of the Science and Innovation division, and is a founding member of the African vaccine manufacturing initiative.
Dr. Francis Collins, director of the National Institutes of Health (NiH) in Bethesda, Maryland, responded by saying: “The African CDC and the African Union (AU) have been outstanding in the way in which you have been mobilising the countries of Africa to respond in a bold way to the Covid-19 pandemic.” Collins also praised governments for laying out actionable plans. He also voiced his and the NIH’s commitment to collaboration via the PAVM.
Collins contextualised this by saying the pandemic highlighted the continent’s dependence on purchasing vaccines from abroad and noted how inequitable this system has been. “The situation will improve markedly in the coming year as the major producers are ramping up production, although right now there’s terrible inequity present,” Collins said. While Collins welcomed the work by those selected to present on the panel to increase Africa’s vaccine manufacturing capacity, he warned that the Covid-19 outbreak would not be the last time this kind treatment would need to be made at scale across the world. The success of the Covid-19 vaccines produced to date was something Collins noted in particular.
“All of these seem to work, in various ways and their precise efficacy and safety are debated, but it is, scientifically, a good position to be in to know that there is science to be working,” Collins said. Collins then posed the question of how a more equitable state of vaccine manufacturing could be achieved to benefit Africa. “I think that’s already under way in places like South Africa. We still need to build the infrastructure and human resources to work with these unique products. What I really want to see is tech transfer from companies to learn while engaging, and we need training so that real innovation and vaccine research can come from African investigators working in this field,” Collins said.
Collins said that National Institutes of Health consulted vaccine manufacturers to share their knowledge and expertise to boost Africa’s capacity, and several stated their commitment to the cause. Collins voiced his encouragement for this as many steps in vaccine manufacturing are developed in-house rather than in the public domain. “We need that willing participation in order to make these kinds of transfer capabilities occur,” he said.
Collins said that a long-term aspect that needed to be considered among global vaccine manufacturers and the NiH was support of the Africa Medicines Agency. “This is going to require a lot of coordination and collaboration, both training and manufacturing methods, researchers to consider other key infections for innovations in manufacture and inclusion of new infectious agents which will further improve the health of Africa.”
Tippo, as moderator, opened the floor to Dr Amadou Sall, who started by discussing training for vaccine manufacturing in Africa. “This has been a great opportunity in getting the right human resources because it’s a strong pillar of vaccine manufacturing and we all have to be conscious of that,” he said. Sall elaborated on the importance of human resources in vaccine manufacturing by saying that it requires a diversity skill like regulation, quality assessment and quality control.
Tippo questioned Sall on where, perhaps, the best opportunities lay in accruing human resources to assist in vaccine manufacturing, citing apprenticeships and internships as possible avenues. “Rather than tackling everything at the same time, we need to prioritise,” said Sall. “The people that can be trained out of university is something that can be fixed locally, but really we may need to tap into the diaspora and we would need to build some sort of curriculum with them.”
Tippo asked Sall if African schools and universities are capable of providing the “raw talent” needed. “We do not have enough universities doing that, but when it comes to apprenticeships, we should leverage vocational education,” Sall said, pointing to people at the end of their high school careers and those beginning university as ideal candidates for training. “This is the type of level where we can get the right crowd,” he said.
Tippo went on to introduce Dr Heba Wali, CEO of vaccine manufacturing firm Vacsera. Wali was encouraged to share the role of research institutions in the development and support of research hubs. “Research and development (R&D) is the backbone of any vaccine and, because of the Covid-19 pandemic, we’ve learned to have very strong R&D,” Wali said. Wali echoed Sall by calling for stronger collaboration between universities and the vaccine manufacturing industry. “We need to encourage academics in the field of research related to the vaccine to be in cooperation with the manufacturer to provide their thoughts from which we can start to develop R&D,” said Wali.
Tippo asked Wali how many research hubs were necessary for Africa. “Africa’s situation is unique because we don’t have many vaccine manufacturers on the continent,” said Wali. “If we had a hub from which we could all share information, I think this would be a good idea because across many countries on the continent you cannot find experience related to the vaccine industry,” she said.
Tippo questioned Wali on the relationship between vaccine hubs and vaccine manufacturers on the continent and potential advice she could share for aspirational vaccine manufacturers. Speaking on how a hub could collaborate with vaccine manufacturers, Wali said that R&D and applied R&D – two separate fields – would assist manufacturers by providing data for upscaled operations.
“Maybe we can also use hubs to promote know-how and inform vaccine producers on how to do that,” she concluded.
[ad_2]
Source link